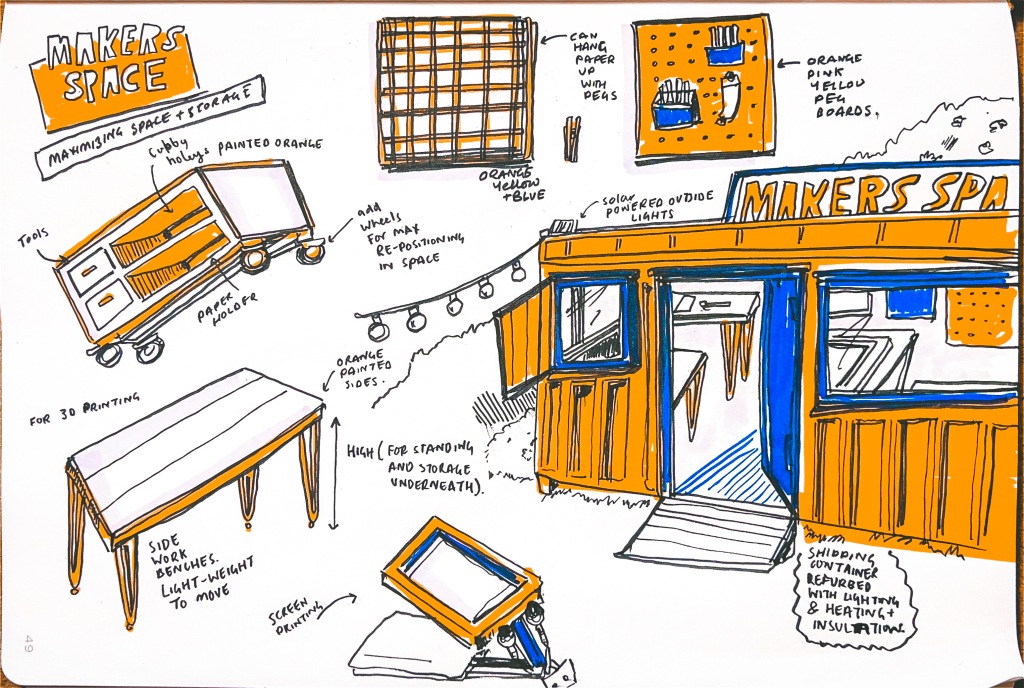
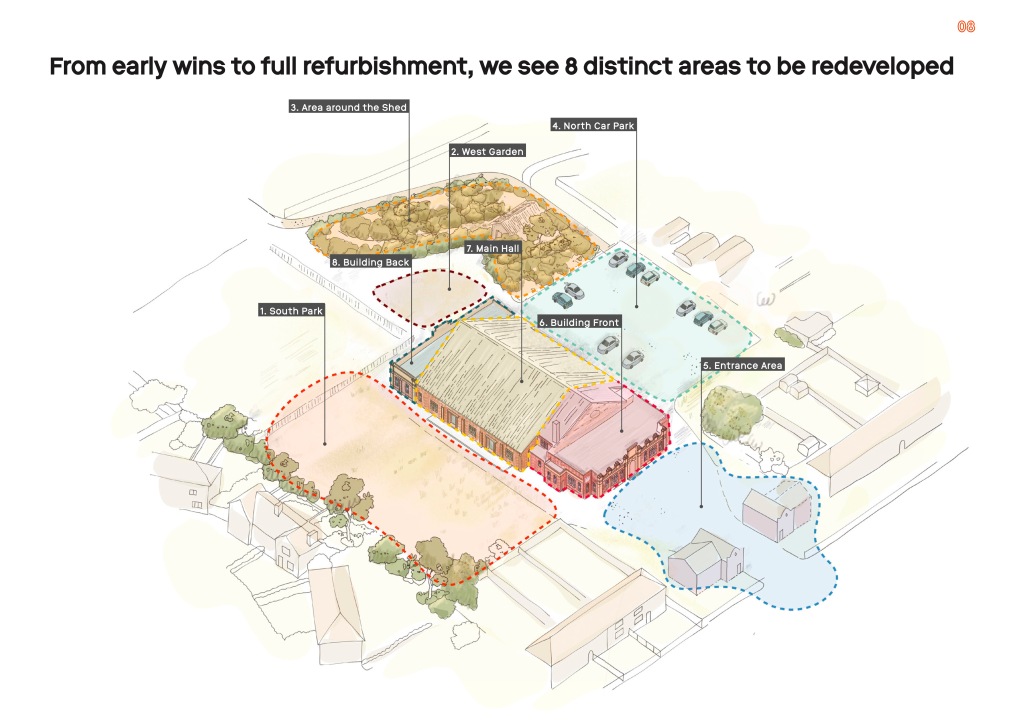
Yesterday I was invited to do a talk in Birmingham, to discuss an artist’s animation video tackling the housing crisis and building on the ideas of video activism and the use of the archive as a revolutionary tool.
It was here that many different areas across England were discussed via the lens of navigating the housing crisis and wanting to get stable living & build a home via council housing.
What was spoken about shocked me a bit. Of course, I academically understand that every place is different. Every ward in Doncaster is different, with its own microscopism of assets and issues. As is the human condition. But I didn’t realized that all the things we do to help people in Doncaster in/access social housing weren’t just done everywhere else?
From helping folks fill out forms for housing, ensuring a more connected approach including social workers etc, getting people a bed for the night who are on the street, to supporting TARA’s and environmental pride etc. I watched videos/heard oral histories of communities having to fight to create a group to help each other fill out forms etc. It was wild. Because it’s so obvious that these things we try and do in Doncaster are vital to a healthier understanding of tenants’ needs. and it’s so vital to building policies, designing new housing, etc, & it needs to be made WITH tenants, of all kinds! Properly. In collaboration.
Now, we still have lots of work to do to get better and the housing landscape in the UK is grim AF adding to our endless challenges which means 100s of people’s housing needs are not being met. BUT we still have these support things in place that aren’t there elsewhere.
This got me thinking about care. And collaboration / co-production. On power, on basic needs and health. I thought a lot about the labour of love in our systems.
If y’all follow me on Twitter, you will know that the past month & a bit feels like all i’ve been doing is a lot of kicking off and getting ground down by inane system-protocol-silo’d behaviours that come across as not connected enough. And as a result, creates poorer outcomes for residents (not person-centred responses) and leaves me feeling burnt out and like – “what’s the point??”. Doesn’t help that I’ve been under the weather too, which drains my usual resilience.
Exhausted on the floor outside a train toilet, from a crazy week, on another too packed & poorly commissioned CrossCountry service (another lack of care)- I was reflecting on all of this. I had also just read the research papers associated with the Guardian’s front page yday: that seeing the same GP = better care outcomes, less hospital admissions, it’s cheaper & keeps people alive longer (25% less risk of death within the next 12 months). Julie & I joked that my GP is adding YEARS to my life. But this is everything we all ALREADY know. But the gov/policy-makers/commissioners are not following our own guidance and evidence. https://www.kingsfund.org.uk/insight-and-analysis/press-releases/radical-refocusing-primary-community-services
All of this swirled inside my head. It made me think of Madeleine Bunting’s “Labours of Love” book when reflecting on our systems of care. For those navigating it and those working and advocating in them.
Within the medical field, a rigid social hierarchy prevails: doctors are tasked with diagnosing and treating, while the responsibility of caring is systematically passed down the ranks, from nurses, HCP & social workers, to healthcare assistants, home caregivers, and countless unpaid individuals such as family members, friends, and volunteers. We see this mirrored in Local Authorities to education systems and beyond.
Despite its profound moral significance and the lofty rhetoric it often accompanies in political discourse, caring remains relegated to a position of low status. There exists a pervasive desire to be perceived as caring without the necessity of engaging in the actual hands-on work of caregiving. This aversion stems from the inherent messiness and discomfort associated with physical care, confronting realities and experiences that many would prefer to avoid.
Madeleine Bunting cites Californian Palliative care doctor B.J. Miller, who describes palliative care as “the art of not running away.” However, in my own experience, acute care is sometimes less challenging than confronting tasks such as managing incontinence, or attending to the complex needs of individuals with severe dementia or disabilities, trying to support people who are homeless & experiencing deep trauma. Additionally, caring for those struggling with addiction, individuals impacted by suicide or abuse, or individuals experiencing psychosis presents its own set of difficulties. Faced with sometimes hostile behaviour, and profound suffering, the natural inclination is to flee. To just accept the first answer that comes back to you. Nevertheless, there are individuals who courageously remain by their side, providing unwavering care and support.
Our determinants of health create the circumstances we face in life, and these deeply influence our need for care. Sadly, those who lack financial resources, social connections, education, or a supportive environment from the very beginning (early help/support = best bang for your ££) are more likely to require assistance.
It is a poignant reminder of the pressing need for empathy and collective efforts to address the growing disparities in our community’s care landscape.
As a councillor, I witness, observe & even experience the Inverse Care Law, eloquently introduced by GP Dr. Julian Tudor Hart in 1971. It unveils a reality where the availability of (health) care is inversely proportional to the urgency of its need. I see the directness of this when I discuss our local casework/issues to other more affluent wards & it’s like 2 different worlds and jobs. These disparities become even more pronounced when market mechanisms dictate the distribution of care.
“Labours of Love” serves as a powerful call to action. Philosopher Michael Sandel aptly points out that our society has transitioned from a free-market economy to a free-market society, inadvertently importing the values and incentives of free markets into social spheres where they do not belong, at all. It is imperative that we reintegrate the values and ethics of care and compassion into our societal framework.
To achieve this, we must cultivate the skill of facing challenges head-on rather than shying away from them. But how do you get a big system to do that? This is my constant question. One that lays heavy between the lines of the moany emails I send.
During moments of privilege, we often pass off tasks that we find tedious, frightening, or gross to others. Yet, it’s crucial to understand that not all caregiving roles are viewed equally. While healthcare professionals caring for the wounded or terminally ill are often highlighted in popular culture, there is a noticeable absence of representation for those dealing with neurological disorders, mental illnesses, or learning disabilities. For our council colleagues who are out doing home visits with people who are deeply frightened or have lots of complexity happening around them. All of this work is often undervalued and not seen as a major skill – when it is – & doesn’t offer the time/space for it happen, rules created by the systems themselves (in response to demand/reduction of resources). Media & organizations depictions of caregiving tend to focus on moments of tranquility and kindness, glossing over the emotional strain and ethical dilemmas that come with looking after others.
This oversight perpetuates a distorted perception of care, failing to acknowledge the significant challenges and sacrifices made by caregivers on a daily basis.
My friend & colleague the other week said, “[organizations] often think that carers are a nice to have, not a necessity.” And it is this friction I find myself rubbing up against & would argue is what is panning out in front of us all across the NHS & beyond.
Care, frequently romanticized or disregarded in media representations, encompasses substantial emotional toil and ethical complexities. The serene depictions of care fall short of capturing the fatigue, self-reproach, isolation and moral conundrums confronted by caregivers, a considerable number of whom are burdened with excessive workloads and inadequate support.
The relational aspect of care, fraught with complexities and emotional demands, poses significant challenges for people and any system that needs to care but isn’t doing it effectively that contributes to burnout of carers (all types of carers, home and work).
When providing care to individuals who have endured trauma (which is a lot of folks), building trust is a gradual process. Initial meetings/communications can be challenging as we all have to navigate boundaries and assess each other’s sincerity. In such encounters, the system is often tempted to encouraging 1-dimensional responses to save time. But end up triggering many involved.
However, I have been where a lot of my residents, who come to me, are. This serves as a reminder of the crucial importance of being fully engaged when faced with people who are distressed or fearful. The relationships formed in these moments of vulnerability are not always easy, as acknowledged by the emails and messages that often begin with, “Sorry for taking up your time…”
At times, I am the only person my residents can get a hold of. I become their key worker by default.
Providing meaningful care to people requires patience and perseverance, with rewards often delayed. Esp. in a system that only half of it understands the necessity to adapt to the needs of a person. However, we must continue to remake our places and investments that allow compassion to bloom. Arthur Frank, a medical sociologist, aptly notes that the disruption of ongoing relationships in caring systems is not merely an organizational issue but a moral failure. It distorts the potential for people to truly connect and support each other.
Again, I think of the work we do in Adult Social Care in Doncaster – a wide and wonderous directorate of spaces and people in the dedication of supporting us all to live the best life and feel cared for. Where we are on the co-production journey with people who know what accessing adult social care in the Donx feels/is like.
We talked at length last month about co-production, caring, collaboration, labour and power. That care is not just a trait; it’s a laborious endeavor deeply influenced by our own experiences of being cared for. It’s demanding work, often undertaken in harsh and risky conditions.
However, this work requires resources, such as time, proper wages, and support, to be sustainable. When individuals who possess a natural disposition for caring lack these resources, they risk burning out as they repeatedly find themselves unable to meet the high standards they set for themselves.
Every day, dedicated professionals in the realm of care are forced to relinquish their roles due to burnout. Exhausted professionals in our systems and organizations, overwhelmed by systems not letting them naturally adapt & treat the needs *of that person/community* & the endless paperwork that comes with it. This shift threatens to squander the innate goodwill and compassion of millions of caring individuals who are expected to continue caring with nothing more than their own inherent kindness to sustain them.
If we truly aim to elevate the status of care, to create more caring systems that connect us all together, and foster a more compassionate society, we must recognize and actively support the immense effort involved in this labour of love.
Material assistance & fair financial expenses, alongside acknowledgment of the challenges faced by caregivers, is essential for cultivating a sustainable culture of care.
I’m proud to see that in Doncaster we are standing in good stead, and need to shout about it more TBH. Sometimes you indeed need to go somewhere else to see stuff that you’re usually looking really closely at. I’m really proud of how caring Doncaster is, both in how we all work together and our fantastic communities.
But I am determined that we will continue to build more infrastructure/freedom to allow care and autonomy and creativity to collide every day, to responddd to people and what they really, truly need. Often that’s time & space & proper listening.
The way forward, I think, is to learn not to run away. To stay and be and figure it out, truly. Together.